Tirzepatide Tablets: Why the FDA-Approved Drug Only Comes as an Injection
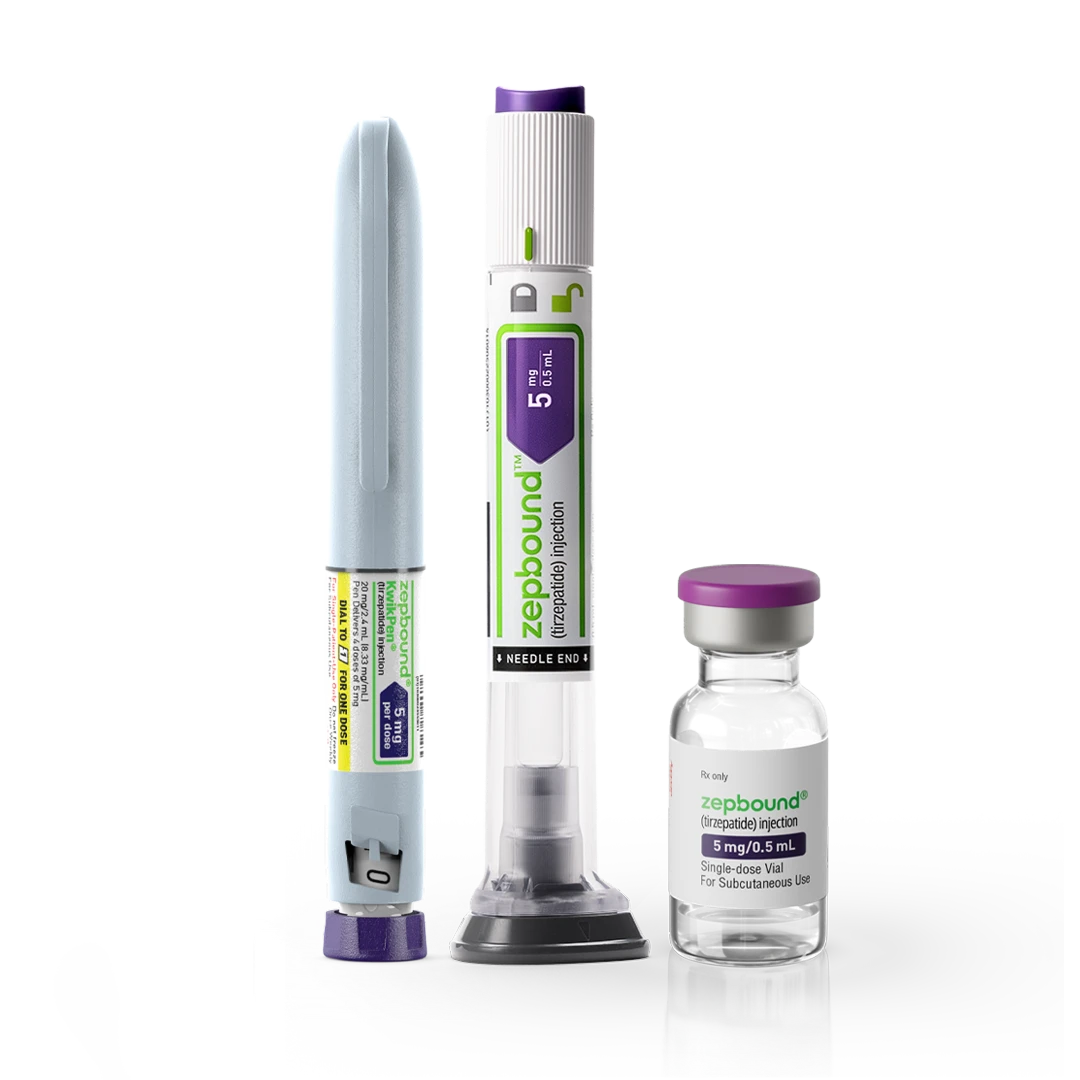
The FDA has approved tirzepatide in six doses (2.5, 5, 7.5, 10, 12.5, and 15 mg), and not a single one is a tablet. Tirzepatide, sold under the brand names Mounjaro and Zepbound, is only approved as a once-weekly subcutaneous injection in prefilled pens or vials.
That hasn't stopped a parallel market from popping up. Compounding pharmacies have started offering "tirzepatide tablets" in sublingual and orally disintegrating forms, pitched as a needle-free alternative. These versions are not FDA-approved, have not been tested in clinical trials, and their safety and effectiveness are largely unknown.
If you're looking at tablet options because you don't want to inject, the practical question is what your real choices are. The short answer: stick with the FDA-approved injection, wait for a different oral drug that's coming through trials, or accept the unknowns of a compounded sublingual. The trade-offs differ a lot.
What's Approved and What's Not
Tirzepatide is a peptide hormone that activates two receptors at once: GIP (glucose-dependent insulinotropic polypeptide) and GLP-1 (glucagon-like peptide-1). The dual action is part of what makes it more effective than older single-target drugs.
The FDA approved it for type 2 diabetes in May 2022 (Mounjaro) and for chronic weight management in November 2023 (Zepbound). Approval was for once-weekly subcutaneous injection only.
The reason peptides like tirzepatide are typically delivered by injection comes down to the gut. Stomach acid and digestive enzymes break down peptide drugs before they can be absorbed. Without protection or a chemical workaround, an oral peptide barely makes it into the bloodstream.
Here's how the available forms compare:
| Form | FDA-approved? | Route | Typical dose | Notes |
|---|---|---|---|---|
| Mounjaro / Zepbound (pen or vial) | Yes | Weekly subcutaneous injection | 5 to 15 mg | Standard of care; covered by SURMOUNT and SURPASS trial data |
| Compounded sublingual or ODT tablets | No | Oral or under the tongue | Varies by compounder | No clinical trial data; FDA has flagged safety concerns |
| Orforglipron (oral, not yet approved) | No (in phase 3) | Daily oral tablet | 6 to 36 mg | Different molecule; GLP-1 only, not GIP |
The Compounded Tablet Problem
When a brand-name drug is in shortage, the FDA allows compounding pharmacies to make versions of the active ingredient. That window opened during the tirzepatide shortage and is what enabled the compounded market. Some compounders started experimenting with sublingual tablets and orally disintegrating tablets (ODTs), pitching them as a needle-free alternative.
There's a real reason these don't have an evidence base. None of the SURMOUNT or SURPASS trials tested oral tirzepatide.
The 85 to 91% of patients who hit at least 5% weight loss in SURMOUNT-1 were all on injections. The 15% to 21% mean weight loss reported with 5 to 15 mg doses applies to subcutaneous delivery, not to whatever dose is theoretically absorbed from a tablet that dissolves under the tongue.
Beyond the missing data, regulators have raised safety concerns about compounded GLP-1 products, including reports of dosing errors. As of late 2024, the agency declared the tirzepatide shortage resolved, which limits the legal grounds for continued compounding. If you're considering a compounded tablet, you're paying for a product that has neither FDA review nor clinical trial evidence behind it.
What Tirzepatide Injection Actually Does
The case for sticking with the approved injection is the data. Tirzepatide has the strongest weight loss results of any drug on the market.
In SURMOUNT-1, the largest tirzepatide obesity trial, 2,539 adults without diabetes received once-weekly tirzepatide or placebo for 72 weeks. Mean weight loss reached 15.0% at 5 mg, 19.5% at 10 mg, and 20.9% at 15 mg, compared with 3.1% on placebo. More than half of participants on the higher doses lost at least 20% of their body weight, a result previously seen mostly with bariatric surgery.
In SURMOUNT-2, which enrolled 938 adults with obesity and type 2 diabetes, tirzepatide produced 12.8 to 14.7% weight loss versus 3.2% on placebo over 72 weeks. A head-to-head comparison with semaglutide (the active ingredient in Wegovy and Ozempic) found tirzepatide produced significantly greater weight loss. A retrospective study of more than 18,000 real-world patients found that those on tirzepatide were more than three times as likely to hit 15% weight loss within a year compared with those on semaglutide.
The most common side effects are gastrointestinal: nausea, diarrhea, vomiting, and constipation. These tend to be mild to moderate and concentrate during the dose-escalation period. Treatment discontinuation rates due to side effects ran 4 to 7% in SURMOUNT trials, similar to placebo at 2 to 3%.
Continuing the medication matters. SURMOUNT-4 randomized people who had already lost weight on tirzepatide to either continue or switch to placebo for 52 more weeks.
Those who continued kept losing weight, reaching about 25% total loss from baseline. Those who stopped regained most of what they had lost. The drug works as long as you keep taking it, and weight tends to return when you don't.
What's Actually Coming Next: Orforglipron
There is a real oral GLP-1 drug in late-stage trials, but it's not tirzepatide. It's orforglipron, a once-daily small-molecule GLP-1 receptor agonist developed by Eli Lilly (the same company that makes tirzepatide).
Orforglipron sidesteps the peptide-digestion problem because it isn't a peptide. It's a small molecule that survives the gut and gets absorbed orally.
In a 72-week phase 3 trial in adults with obesity, orforglipron at 36 mg produced 11.2% weight loss versus 2.1% on placebo. About 18% of participants on the highest dose lost at least 20% of their body weight.
That's meaningful, but it's not tirzepatide-level. Tirzepatide injection produces meaningfully more weight loss than orforglipron at the doses tested, likely reflecting tirzepatide's dual GIP/GLP-1 mechanism versus orforglipron's GLP-1-only action. The pipeline also includes triple agonists like retatrutide, which targets GIP, GLP-1, and glucagon receptors and produced 24.2% weight loss at 12 mg in a 48-week phase 2 trial.
If orforglipron is approved by the FDA, it would be among the first oral GLP-1 drugs cleared for weight loss. But it won't be a tirzepatide tablet. The molecule is different, and the efficacy ceiling is lower.
What This Means If You're Looking at GLP-1 Options
The bottom line: there is no FDA-approved tirzepatide tablet, and the compounded versions don't have clinical evidence behind them. If you want the weight loss results from the SURMOUNT trials, you need the injection. If you want an oral option backed by phase 3 data, orforglipron is coming, but it's a different drug with somewhat smaller effects.
Instalab's GLP-1 Program ($99) pairs you with a licensed physician who reviews your eligibility, prescribes brand-name GLP-1 medications including Zepbound and Wegovy, and adjusts your dose based on lab results and tolerability over time. The medication is shipped from the manufacturer, not compounded. The program is designed for people who want the FDA-approved drug with ongoing clinical oversight rather than the compounded alternatives sold as tablets or sublingual products.
If you're already comfortable injecting once a week, the data favors sticking with the approved product. If a needle is a non-starter, waiting for orforglipron may be the better play, even though the trade-off is somewhat less weight loss in exchange for an oral pill.
Prescribed by a licensed physician. Sent to your pharmacy.

